
The second category is Neurological TOS, which is broken down further into true and symptomatic TOS.The first category is V ascular TOS, which includes arterial and venous and accounts for ~ 5% of all presentations.In the current research trials, thoracic outlet syndrome is being classified into the following categories: Classification of Thoracic outlet syndrome Below are some of the key features of TOS that I found consistently throughout the literature to be present in this condition. Many patients may present with a cluster of arterial, venous, neurogenic and pain symptoms and diagnosis relies on clinical reasoning of the assessing therapist. Diagnosis will rely heavily on physical examination and collection of objective asterisk signs for reproduction of symptoms. And, the third point of controversy is about the lack of a clear definition of the clinical presentation of TOS. The f irst point of controversy is that the definition does not specify where or what or how compression occurs. The second point of controversy revolves around the diagnosis of symptomatic TOS, where no radiological or electrophysical abnormalities can be detected and the pathological cause for symptoms is unknown. Let's take a look at these points of controversy in closer detail. 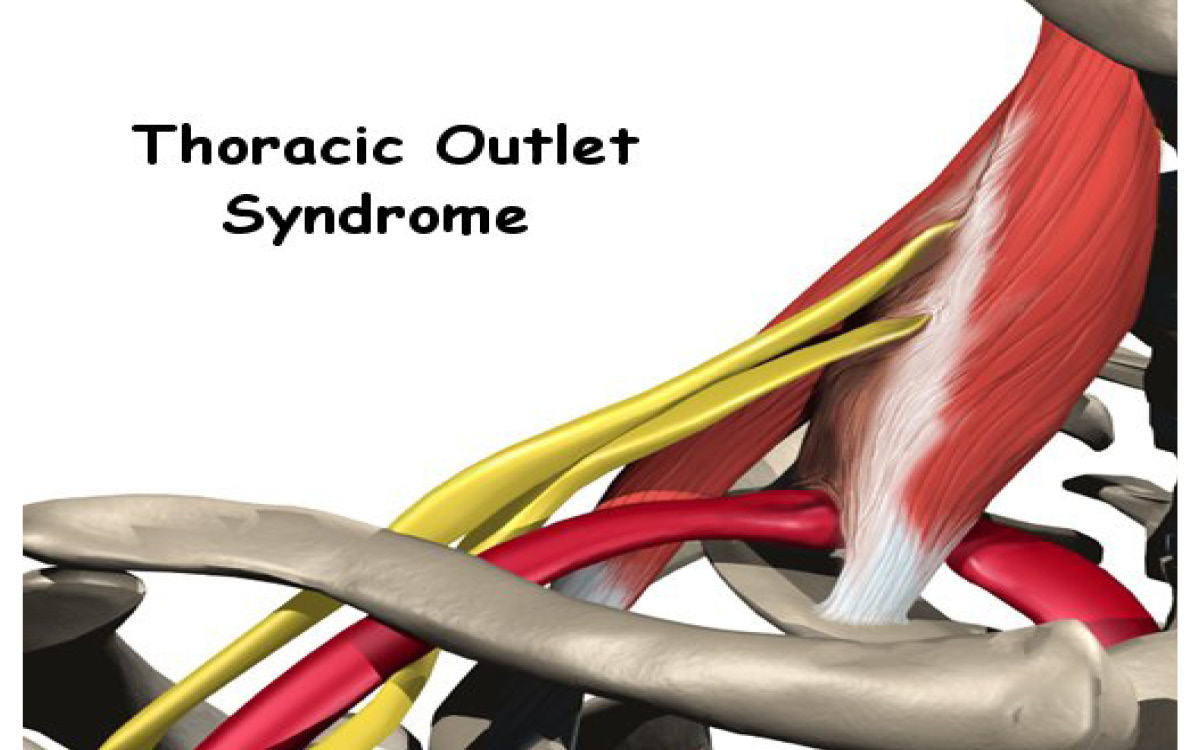
If you are reading about TOS you might noticed that there is always an element of controversy about it's definition, diagnosis and treatment. This leads to poor study results due to the heterogeneity of the study population. When reviewing literature in the topic of TOS keep an open mind that the condition itself and subject population are often poorly defined and vary enormously between studies. Thoracic outlet syndrome was first described in 1927 by Adson and colleagues and known at this time as scalenus anticus syndrome. The formal term that most authors refers to as Thoracic outlet syndrome was derived by Peet and colleagues in 1956. The term thoracic outlet syndrome describes a cluster of symptoms sitting on a continuum ranging from intermitted postural symptoms to severe/permanent neurological/vascular deficits. (Hooper, Denton, McGalliard, et al., 2010a Sanders, Hammond, & Rao, 2007 Watson, Pizzari, & Balster, 2009, Kaczynski, & Fligelstone, 2013) In conclusion, symptoms of FP and OH associated with brachial plexus compression is due to cervical plexus compression by SA muscle, and symptoms can be relieved by resection of the SA.Thoracic outlet syndrome (TOS) is a syndrome/condition that encompasses cluster of upper extremity symptoms which are due to compression of the neurovascular bundle by various structures in the area just above the first rib and behind the clavicle. The three most common regions where compressions is thought to occur is the intrascalene triangle, the costoclavicular triangle and the subcoracoid space. OH was completely relieved in 81% and partially relieved in 13% of the patients. Postoperatively, for those patients with neck pain, with or without facial pain, 75% were completely relieved, 18% were partially relieved. It was found that 25% of the patients had FP and that 50% had OH. To evaluate this, a consecutive series of 32 patients who had resection of the SA between January 2004 and December 2007 were evaluated to determine prevalence of FP and OH, and the extent to which these symptoms were relieved postoperatively after SA resection. Furthermore, it was hypothesized that tension on the origin of this muscle from the transverse cervical processes causes compression of the occipital nerves. It was hypothesized that SA contraction compresses the cervical plexus as it exits deep to this muscle. With the realization that scalenus anticus (SA) contraction is the primary source of brachial plexus compression, it is possible to understand the occurrence of both FP and OH in this syndrome. 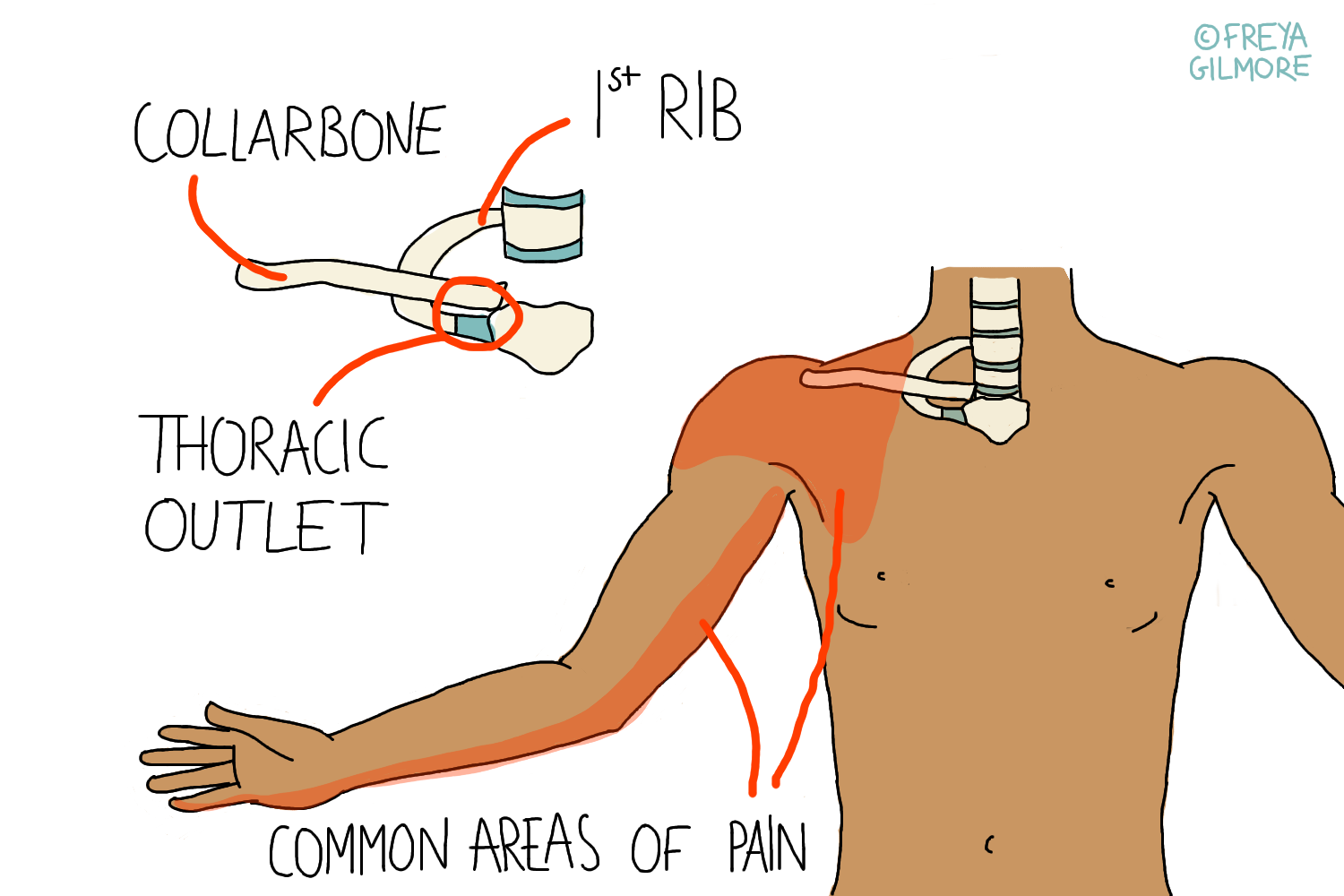
Among the sources for confusion related to brachial plexus compression in the thoracic inlet are the name for this clinical entity (thoracic outlet syndrome) and the fact that some of its associated symptoms occur outside the upper extremity, such as face and neck pain (FP) and occipital headaches (OH).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
